HEMODYNAMIC MONITORING AT YOUR FINGERTIPS
Continuous non-invasive blood pressure, cardiac output and fluid management for moderate and low-risk surgery
CNAP® Monitor
CNAP® Monitor provides advanced hemodynamic information from the non-invasive reusable CNAP® finger sensor. It supports your Goal Directed Therapy whenever an arterial line is not indicated. Patient-friendly, easy-to-use, cost-efficient.

PREVENT HYPOTENSION
Perioperative complications such as acute kidney injury (AKI), myocardial injury (MCI) and cardiac complications are related to hypotension(1) . Using continuous non-invasive blood pressure monitoring can help to prevent intra-operative hypotension.

REDUCE COMPLICATIONS
Reduce postoperative complications up to 34% and infections up to 61% even in low & moderate-risk surgeries applying individualized Goal Directed Therapy.(2)

IMPROVE OUTCOME
MOST POPULAR NON-INVASIVE BLOOD PRESSURE & HEMODYNAMICS
You are currently viewing a placeholder content from Vimeo. To access the actual content, click the button below. Please note that doing so will share data with third-party providers.
More InformationUnique combination of non-inasive & continuous
Your choice for non-invasive hemodynamic monitoring
CNAP® Monitor offers a unique set of parameters to support your daily routine – all non-invasive & continuous allowing for perioperative fluid management even in low and moderate-risk surgeries and patients.
CNAP® Monitor provides smart features to make hemodynamic monitoring easy:
- High-fidelity CNAP® blood pressure waveform
- Easy setup through reusable CNAP® finger sensor
- Quick & time saving compared to invasive arterial blood pressure
- Automatic calibration to gold standard with integrated NBP (for highest accuracy)
- Alternative calibration modes to external reference values (BP, CO)
- Easy interfacing with your patient monitor
All parameters are provided by the CNAP® finger sensor.
- Finger blood pressure: CNAP® waveform, SYS, DIA, MAP, Pulserate
- Upper arm NBP: SYS, DIA, MAP
- Advanced hemodynamics (CNAP® HD): CO, CI, SV, SI, SVR, SVRI
- Dynamic fluid response parameters: PPV, SVV
Most popular finger blood pressure method for non-invasive continuous hemodynamics.
More than 1,000 peer reviewed publications prove that the CNAP® technology is the most popular method of measuring continuous non-invasive finger blood pressure and hemodynamics in research and clinical routine.
More than 5,500 customers worldwide and leading global partners trust in our over 20 years of experience in noninvasive hemodynamic monitoring.
Non-invasive continuous blood pressure, cardiac output, stroke volume and additional advanced hemodynamic markers are provided from your fingertips using CNAP® technology.
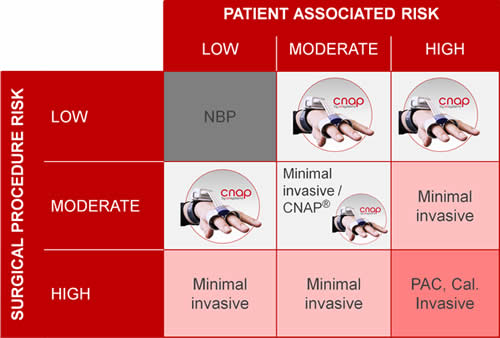
Most popular applications
Where non-invasive continuous technology improves the outcome.
The CNAP® finger sensor offers a unique combination of non-inasive and continuous blood pressure, cardiac output and dynamic fluid response parameters.
Therefore the CNAP® Monitor is the ideal tool for personalized fluid management in low and moderate risk cases.
“Full characterization of fluid responsiveness requires consideration of the type, amount and timing of fluid as well as the expected change in stroke volume. The best method of measuring fluid responsiveness is a continuous or rapidly repeatable measure of stroke volume.[…] Alternative methods for predicting fluid responsiveness include stroke volume variation (SVV), pulse pressure variation (PPV), systolic pressure variation (SPV), and (in certain mechanically ventilated patients) end-expiratory occlusion test and respiratory systolic variation test.” (4)
Intraoperative hypotension may cause serious complications such as myocardial injury, acute kidney injury, and death. In the postoperative period, hypotension is common, but remains widely undetected in general care floor settings, and is independently associated with myocardial injury and mortality . “Critical care patients are especially sensitive to hypotension, and the risk appears to be present at blood pressures previously regarded as normal.” (5)
Thus, if detected early enough, complications due to hypotensive episodes could be reduced or even avoided.
“Understanding intraoperative events that predict morbidity and mortality could improve perioperative care in surgical patients by preventing events or initiating treatments after adverse events.” (1)
Non-invasive CNAP® Monitor enhances perioperative monitoring by providing continuous blood pressure and advanced hemodynamic information even in low and moderate-risk surgeries. Continuous blood pressure monitoring enables hypotensive phases to be detected earlier compared with intermittent NBP monitoring, which helps to improve patient safety.(6)
A rapid change of hemodynamic status requires daily examination for individualized treatment, using functional hemodynamic tests such as Passive Leg Raising (PLR), End Expiratory Occlusion Test (EEOT) and Mini Fluid Challenge (MFC) at the bedside.
Furthermore, the complex interaction of respiration, right ventricular (RV) function and other cardiovascular factors creates a therapeutic conflict between conservative fluid management vs. hypovolemia from an early stage of COVID-19 (too wet vs. too dry).
CNAP® Monitor 500 HD provides essential feedback for functional hemodynamic tests to direct volume expansion in patients without invasive line indication:
- Supports healthcare professionals in educated hemodynamic management decisions
- Helps to guide conservative fluid management while preventing hypovolemia
- Simplifies daily examination and individualized treatment
- Quick and easy application with minimal training required
- No burden to patients
- Supports healthcare professionals in daily clinical routine
- Early recognition to prevent deterioration
CNAP® Monitor is an easy-to-use tool to upgrade your research with full hemodynamics. It is highly valued for:
- Providing continuous blood pressure and advanced hemodynamics from one sensor
- Delivering reproducible results
- Simple interfacing
- Being clinically proven and validated
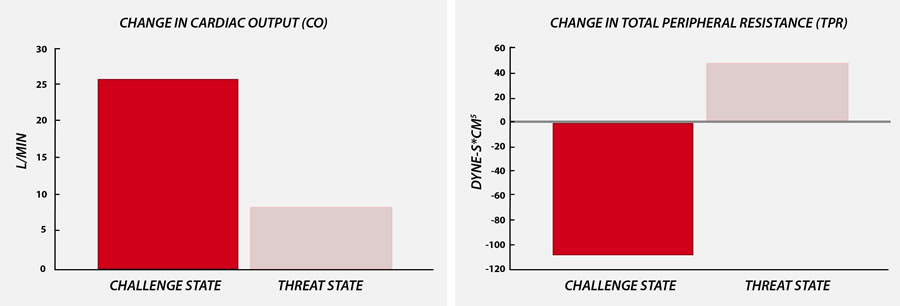
EXAMPLE – application in psycholophysiology:
Blood pressure, cardiac output and systemic vascular resistance are important correlates for assessing challenge and threat in Psychophysiological Research. (7,8,9)
adapted from Blascovich et al. (9)
Unique Products
Unique Customers
Our mission is to meet the needs of our customers and make their daily clinical routine or scientific work easier. The steadily increasing number of loyal customers confirms the trust in our technologyfirms the trust in our technology.




FREQUENTLY ASKED QUESTIONS
For additional questions contact us!
The continuous values come from the CNAP® finger sensor. The internal NBP cuff just provides reference values for calibration to brachial pressure at heart level.
Numerous studies across various surgical patient populations show a weighted average Bias +/- SD for mean blood pressure (MAP) of – 0,29 +/- 7,87 mmHg. (10)
Systolic , diastolic and mean blood pressure provided by CNAP® fulfill the blood pressure standard (ISO 81060-2) of BIAS 5mmHg and SD 8 mmHg.
- CNAP® could provide continuous blood pressure non-invasively in some patients, where the invasive measurement is used for BP monitoring only, without the need for blood-gas sampling
- CNAP® could be used in addition to invasive blood pressure monitoring to provide advanced hemodynamic parameters such as SV, CO and SVR.
The CNAP® HD applies a pulse contour analysis (PCA) algorithm to the non-invasive blood pressure signal (CNAP® finger sensor). The PCA calculates stroke volume (SV) from the BP waveform. Cardiac output (CO) is calculated from SV times heart rate (HR).
- CNAP® measures continuously at the finger artery.
- Calibration to brachial pressure is achieved with an integrated NBP cuff.
- After repositioning of the patient, the fingers or the hand you have to use the NBP to recalibrate the system (eliminating hydrostatic offset).
- Yes, CNAP® can be used during exercise tests, as far as the hand applied with the CNAP® finger sensor is not clenched to a fist and the sensor is kept in a constant position in relation to the heart (constant hydrostatic offset).
- However, finger movement causing changes in the setup of the finger sensor will result in artifacts.
- Use an arm sling or armrest to keep the arm in a constant position.
HEMODYNAMIC MONITORING AT YOUR FINGERTIPS
Continuous non-invasive blood pressure, cardiac output and fluid management for moderate and low-risk surtgery.
References:
(1) Kurz, A., Turan, A., Rodseth, R. N., Cywinski, J., Thabane, L., Ph, D., & Sessler, D. I. (2013). Relationship between Intraoperative Mean Arterial Pressure and Clinical Outcomes after Noncardiac Surgery. Anesthesiology, (3), 507–515.
(2) Benes, J., et al. (2015). Fluid management guided by a continuous non-invasive arterial pressure device is associated with decreased postoperative morbidity after total knee and hip replacement. BMC Anesthesiology, 15(1), 148. doi:10.1186/s12871-015-0131-8
(3) Grocott, M. P. W., Dushianthan, a, Hamilton, M. a, Mythen, M. G., Harrison, D., & Rowan, K. (2013). Perioperative increase in global blood flow to explicit defined goals and outcomes after surgery: a Cochrane Systematic Review. British Journal of Anaesthesia, 111(4), 535–548.
(4) Martin GS, Kaufman DA, Marik PE, Shapiro NI, Levett DZH, Whittle J, MacLeod DB, Chappell D, Lacey J, Woodcock T, Mitchell K, Malbrain MLNG, Woodcock TM, Martin D, Imray CHE, Manning MW, Howe H, Grocott MPW, Mythen MG, Gan TJ, Miller TE. Perioperative Quality Initiative (POQI) consensus statement on fundamental concepts in perioperative fluid management: fluid responsiveness and venous capacitance. Perioper Med (Lond). 2020 Apr 21;9:12. doi: 10.1186/s13741-020-00142-8. PMID: 32337020; PMCID: PMC7171743.
(5) Ruetzler K, Khanna AK, Sessler DI. Myocardial Injury After Noncardiac Surgery: Preoperative, Intraoperative, and Postoperative Aspects, Implications, and Directions. Anesth Analg. 2020 Jul;131(1):173-186. doi: 10.1213/ANE.0000000000004567. PMID: 31880630.
(6) Nicklas JY, Beckmann D, Killat J, Petzoldt M, Reuter DA, Rösch T, Saugel B. Continuous noninvasive arterial blood pressure monitoring using the vascular unloading technology during complex gastrointestinal endoscopy: a prospective observational study. J Clin Monit Comput. 2019 Feb;33(1):25-30. doi: 10.1007/s10877-018-0131-6. Epub 2018 Mar 20. PMID: 29556885.
(7) Kirby, L. D., & Wright, R. A. (2003). Cardiovascular correlates of challenge and threat appraisals: A critical examination of the Biopsychosocial Analysis. Personality and Social Psychology Bulletin, 7, 216-233.
(8) Tomaka J, Blascovich J. Effects of justice beliefs on cognitive appraisal of and subjective, physiological, and behavioral responses to potential stress. J Pers Soc Psychol. 1994 Oct;67(4):732-40. doi: 10.1037//0022-3514.67.4.732. PMID: 7965617.
(9) Blascovich J, Mendes WB, Hunter SB, Salomon K. Social “facilitation” as challenge and threat. J Pers Soc Psychol. 1999 Jul;77(1):68-77. doi: 10.1037//0022-3514.77.1.68. PMID: 10434409.
(10) Weighted Average across 15 studies with CNAP® in more than 1,000 patients in OR and ICU settings. (Jeleazcov 2010, Hahn 2012, Biais 2010, Wagner 2015, Kako 2013, Tobias 2014, Ilies 2015, Ilies 2012, Smolle 2015, Lakhal 2016, Dewhirst 2013, Kumar 2015, Jagadeesh 2012); detailed list of references available at CNSystems.